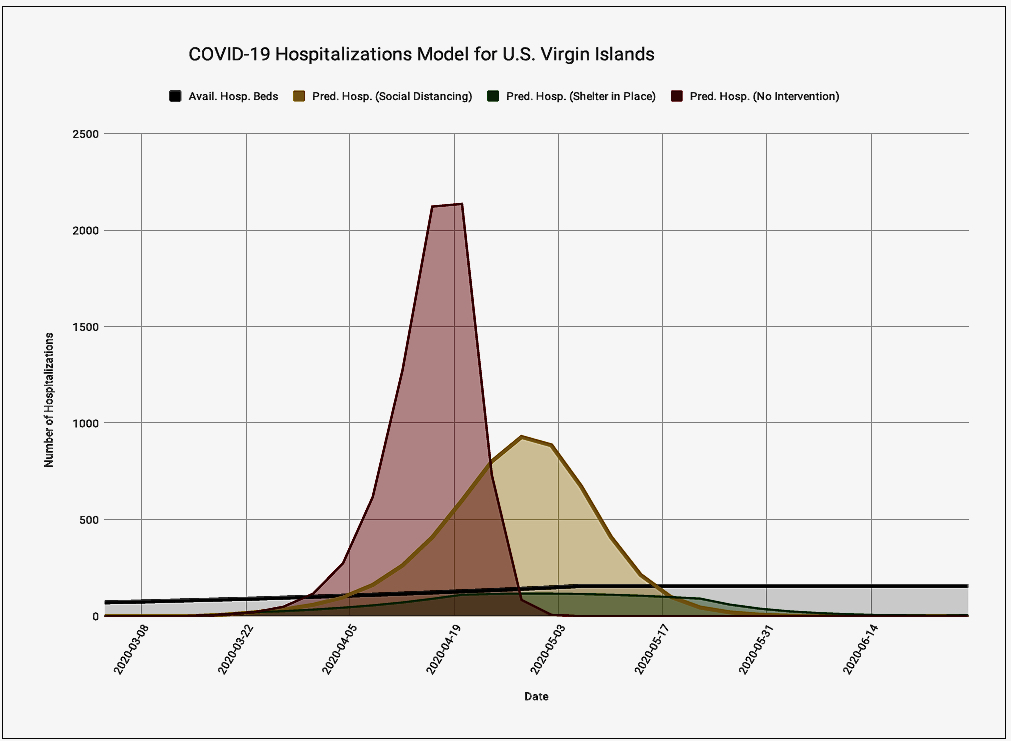
If V.I. residents “shelter in place” as Gov. Albert Bryan Jr. directed and we are lucky, a peak of 117 or so COVID-19 patients may need hospitalization at one time, V.I. Health Department officials project.
But if too many people try to go on about their lives and go out and interact with others, we may exceed capacity.
Roughly 20 percent of those infected require hospitalization and more than 1 percent die. Those figures appear moderately constant – as cases increase, hospitalization, ventilator and mortality rates increase at about the same rate.
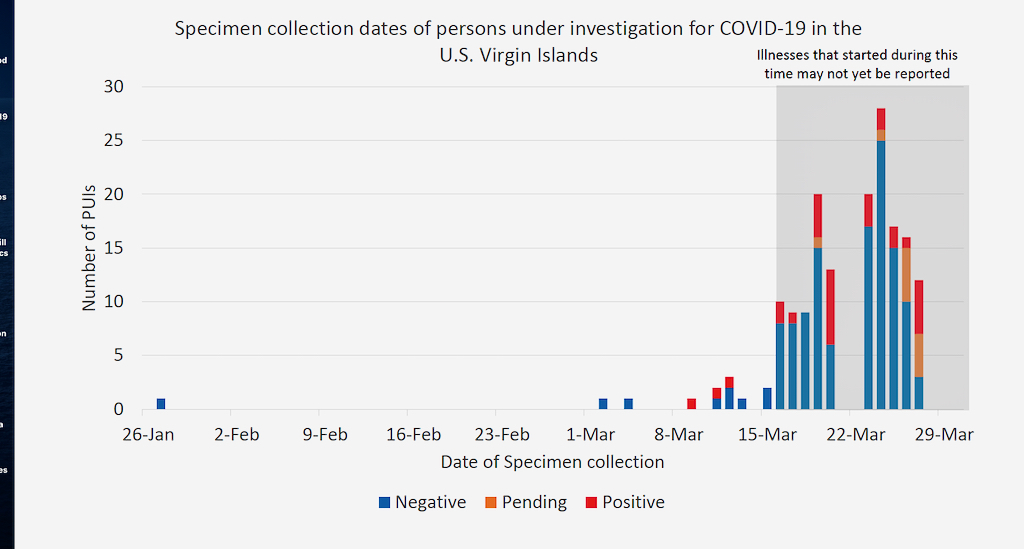
Right now, infections and fatalities in the U.S. as a whole are doubling every three days. On March 20, six Virgin Islanders were confirmed positive for COVID-19. As of April 2, 13 days later, the count stands at 33 with 30 already recovered.
If it spread in the USVI at the same rate as the country as a whole, doubling every three days, and nothing happened to sharply bend it downward, we would see tens of thousands infected and thousands requiring hospital beds – levels far beyond the territory’s capacity.
Fortunately, USVI numbers are not doubling at the rates of most U.S. states.
“The good news is we have very limited community spread, which means ‘shelter in place’ is working,” territorial epidemiologist Esther Ellis said in an email.
She indicated the prospects for a relatively softer landing are good, so long as everyone stays at home for the next two weeks, barely interacting with anyone else outside the home, keeping social distance of six feet when out getting groceries or other unavoidable necessities.
The less we all go out, the better.
According to Ellis, mathematical models suggest if we continue to strictly “shelter in home” “the most hospitalized at any one time would be 117 people within the territory during 4/28 and 5/2.”
At the same time, if we only sort of avoid social contact and sort of maintain social distancing, nearly a thousand people might require hospitalization at the epidemic’s peak, according to their projection (the yellow line on the graph). And if we just carried on as usual, more than 2,000 could require hospitalization.
Assuming all goes well, or as well as can be, and 117 people require hospitalization, the V.I. hospital system will be strained.
Based on past budget testimonies, the territory has around 250 regular hospital beds, with 169 at Schneider Regional Medical Center on St. Thomas and 80 at Gov. Juan F. Luis Hospital on St. Croix. A dozen additional intensive care beds were just added to JFL, so perhaps there are as many as 265 beds. Schneider officials said recently that 60 beds are usually occupied. With a similar population size, JFL should have a similar number of beds occupied. So, optimistically, perhaps 165 beds are actually available, without some expanded capacity.
Schneider officials say they are working to increase capacity to meet the anticipated increased need for inpatient care due to the COVID-19 pandemic by up-fitting an existing unused patient care unit within the facility. This new unit will reportedly be specifically engineered with negative pressure and isolation rooms to accommodate patients affected by COVID-19. JFL officials did not respond to requests for similar information.
If patient numbers remain in that 117 range, there are beds for them. If they swell to a thousand at once, there are not, without dramatic steps to find several hundred additional beds both on St. Thomas and St. Croix.
Officials have said they are working on additional capacity, but there has not yet been a public announcement naming any specific facility of such size.
“I can’t speak to exactly how many beds each facility has right now. I do know this number is increasing as we go along because we are building capacity to be able to handle more hospitalizations,” Ellis said.
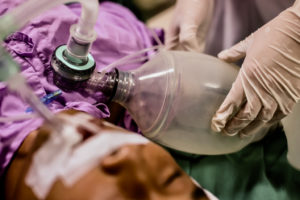
Another piece of good news; unlike some areas, the USVI seems to have enough ventilators. Hospitals in New York are facing a shortage that threatens to force them to share ventilators and to decide which patients do not get them. Ellis confirmed that about six percent of those hospitalized with COVID-19 may require a ventilator. At the low-end projection of 117 patients at once, that would mean about seven Virgin Islanders may need ventilators at once.
“We have a total of 107 ventilators in the territory; 27 reusable and 80 one-time usage,” Ellis said.
Even at the higher level of 900 to 1,000 patients at peak, no more than 60 or so would be needed, so that’s enough for a single surge. And Health Commissioner Justa Encarnacion has said another 50 are on order, though it is unclear if they will arrive before the peak of the epidemic.
So, everyone should continue to shelter at home, wash your hands, keep social distance and so forth, and hold on tight for the next month. Health officials say anyone experiencing symptoms – including a persistent cough, fever and shortness of breath, should self-quarantine and contact the Health Department by telephone at 340-712-6299 or 340-776-1519.











